Search
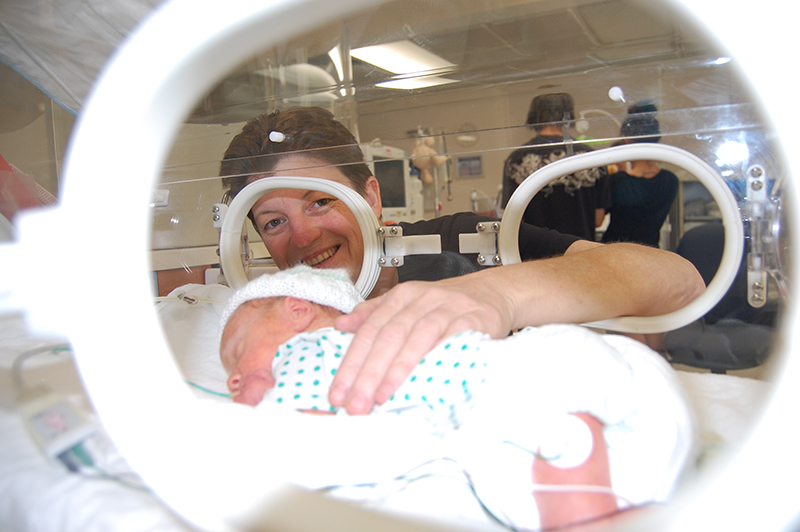
The Chronobiology team works to understand the factors that contribute to poor lung and heart function in newborn infants and find ways to prevent heart and lung disease.
Preterm infants are often vitamin A deficient, and vitamin A has functions that could mitigate the processes that lead to bronchopulmonary dysplasia. Therefore, supplementation of preterm infants with vitamin A to reduce the risk of bronchopulmonary dysplasia makes inherent sense.
Data on static compliance of the chest wall (Ccw) in preterm infants are scarce. We characterized the static compliance of the lung and Ccw to determine their relative contribution to static compliance of the respiratory system in very preterm infants at 36 wk postmenstrual age. We also aimed to investigate how these compliances were influenced by the presence of bronchopulmonary dysplasia and impacted breathing variables.
Inflammation and oxidative stress play a key role in the development of bronchopulmonary dysplasia (BPD), possibly contributing to persistent respiratory morbidity after preterm birth. We aimed to assess if inflammatory markers were elevated in exhaled breath condensate (EBC) of infants born very prematurely (< 32 weeks gestation) at 12-16 corrected months of age, and if increased levels were associated with BPD diagnosis and respiratory morbidity.
The importance of lung recruitment before surfactant administration has been shown in animal studies. Well designed trials in preterm infants are absent. We aimed to examine whether the application of a recruitment manoeuvre just before surfactant administration, followed by rapid extubation (intubate-recruit-surfactant-extubate [IN-REC-SUR-E]), decreased the need for mechanical ventilation during the first 72 h of life compared with no recruitment manoeuvre (ie, intubate-surfactant-extubate [IN-SUR-E]).
Preterm infants have immature control of breathing and impaired pulmonary gas exchange. We hypothesized that infants with bronchopulmonary dysplasia (BPD) have a blunted ventilatory response and peripheral oxygen saturation (SpO2 ) instability during a hypoxic challenge.
A Cochrane 2016 review indicated cycled light might benefit neonatal health in hospital. We systematically reviewed chronobiological factors for neonatal health in hospital units, identifying 56 relevant studies on light-dark cycles, feeding, noise, massage therapy, rooming-in, incubators vs. cribs, neonatal units vs. homes, and time-of-day of birth. Empirical evidence for benefits from chronobiology is weaker than expected, including light.
Normal in utero lung development and growth rely upon the expansion of airspaces and the controlled efflux of lung liquid into the amniotic space. Infants with congenital diaphragmatic hernia (CDH) also have lung hypoplasia due to occupation of the chest cavity by the stomach and bowel and, in the most severe cases, the liver. Balloon tracheal occlusion reduces the severity of lung hypoplasia in fetuses with CDH but increases the risk of premature birth.
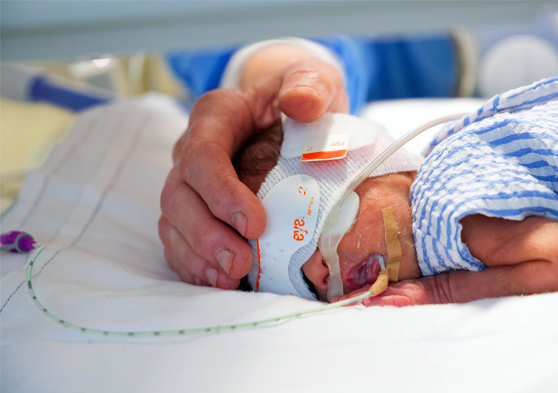
The CIRCA DIEM study is a multicentre, prospective, open, blinded end-point (PROBE) parallel controlled study which aims to compare long term neuro-developmental outcomes of premature babies cared for in a cycled environment to premature babies who receive routine care in a non-cycled environment.

The CIRCA DIEM Study is a multicentre study, involving several different hospital sites across Australia. Here, you can find out more about which hospitals recruit babies into the CIRCA DIEM Study.
